Children’s Pelvic health
Every child has a unique ‘internal environment’, which is in turn responding to their external environment in every moment of every day, as they develop and grow in the world. Children have their own perspective, and this may be different to that of their parents/caregivers. As specialists working in the field of pelvic health, we aim to hear both perspectives and we consider this relationship between parent and child as vital in healing bladder and bowel problems.

Toilet training
Many parents struggle to know when and how best to toilet train their child, and report problems such as frequent accidents, pooing in nappies but not in the toilet, and holding on to poos. Children need to feel safe in order to toilet train and empty both their bladder and bowel effectively. Poor toilet training can lead to problems with bladder and bowel control for children as they develop. For example, reward/punishment programs can promote poor habits such as straining; they can also create fear around toileting as children feel pressure to “perform” and please their parents.
A child who fears the toilet will tense their pelvic floor muscles unconsciously, resulting in incomplete emptying. This can set up problems with bladder and bowel control that become frustrating and distressing for children and their families. Stay tuned for our unique course on healthy toilet training for toddlers.
Daytime wetting
Around 30% of all four year olds will have ‘wee accidents’; this reduces to around 5% of all six year olds, and declines further still in teenagers (approximately 3%). Regardless of age, urinary incontinence can be extremely distressing for children and teenagers, and can result in a range of behaviours from reduced fluid intake, to breakdown of family relationships with denial, secrecy, oppositional defiance and high anxiety. Our sensitive approach to assessing and managing daytime wetting in children aims to restore children’s dignity and feeling of wellbeing.
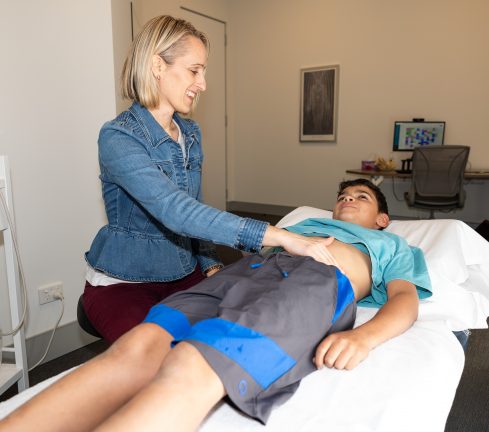
We value hearing from children and often work one to one as both children and parents feel safe for us to do so. We aim to gently help children understand and feel the processes happening within their body, and move towards healing bladder function.


Bedwetting
Around 5-10% of 6-7 year olds, 3% of 10 year olds and 1-2% of 15 year olds wet the bed while sleeping at night. Whilst the incidence reduces with age, the stress, anxiety and life impact for children, teenagers and families, does not. It is unlikely that children ‘grow out of it’ as was once thought. Instead, children adapt in order to manage and/or hide their symptoms. This can significantly increase anxiety around participation in usual actives like sleepovers, school trips, combined family holidays and later, personal relationships. It is likely that children ‘carry’ some degree of bladder and/or sleep dysfunction into adulthood unless treated.
Standard treatments for bedwetting in children have included alarm therapy and medication, however for many children, they have limited benefit. In contrast children who wet the bed may have other symptoms e.g. daytime bladder and/or bowel dysfunction that ‘hide’ and when left untreated can cause other problems. At Consano, our approach is different. We seek to find the underlying ‘drivers’ for bedwetting, and consider all aspects of a child’s life as relevant in this restorative journey.
Constipation
Chronic constipation is the most common bowel problem in children, affecting around 10% of children worldwide. There are a variety of causes and contributing factors to constipation in children, including poor toilet training, stool withholding, poor diet and/or fluids, poor eating habits, limited physical activity, poor toilet habits, altered gut health and unmet emotional needs. A child who doesn’t feel safe, or is in pain, will unknowingly tense their abdominal and pelvic floor muscles, contributing to the holding-in and dehydration of bowel contents.
In some children, the bowel is also much slower to move content along (slow transit constipation) – more common in children with joint hypermobility. At Consano we take a ‘systems’ approach to healing problems related to the bowel, and consider biological, nutritional, emotional, myofascial, mechanical, postural, psychological and social contributors. Our focus is on hearing the needs of the individual child and supporting them to restore their gut health in collaboration with their primary caregivers. We are sensitive to the psychological trauma often associated with typical treatments for constipation and seek to provide a holistic pathway to normal toileting for each child.
Constipation in children usually includes at least two of the following symptoms:
- Regular straining
- Regular hard/lumpy poos/pebbles
- Not knowing the feeling of emptying
- Fewer than three bowel movements per week
- Bowel movements requiring assistance to empty (e.g. suppositories)
- Withholding manoeuvres

Soiling
Soiling of faeces (faecal incontinence, sometimes called encopresis) is an enormously distressing problem for children and families. Sometimes soiling is the result of ‘overflow’ due to a blockage, such as constipation or faecal impaction. Still other times, soiling may be the result of a food allergy/intolerance, or excessive laxative therapy. Difficulty with feeling the arrival of a poo in the rectum and/or the muscles within the anus, make it extremely challenging for children to get to the toilet in time.
Alternatively, incomplete emptying on the toilet can result in soiling after toilet visits. Some children are aware of their soiling; many are not aware at the time. The shame associated with soiling is felt deeply by children and may present outwardly as behaviours such as hiding dirty underwear, lying, anger, avoidance of going to the toilet, tantrums or oppositional defiance. These behaviours are frustrating for caregivers and children are often judged for them, which serves to deepen their sense of shame and loss of control over their body. After careful assessment, at Consano we begin the journey with education. We gently help children to understand and feel the processes happening within their body, and move towards healing bowel function and restoring wellbeing.
Pelvic and abdominal pain
Pain in the abdomen or pelvic region without an obvious medical cause (eg appendicitis, gastroenteritis) is sometimes labelled ‘functional’. This may include pain after eating, pain during or after bowel evacuation, bladder pain, abdominal wind/bloating, prolonged or recurrent pain after surgery, pain with no apparent trigger, pain around the opening of the vagina (vulva) in girls or scrotum and testes in boys. Sometimes children or teenagers are diagnosed with abdominal migraine, abdominal pain syndrome or pelvic pain syndrome. Sometimes a fall onto the tailbone or saddle area can result in ongoing pain and tension in the surrounding tissues, including the pelvic floor muscles.
Sometimes trauma is the underlying driver of ongoing pain. Our sensitive and holistic approach extends to children and teenagers with symptoms of pelvic and/or abdominal pain. We help young people and families to understand pain from myofascial (connective tissue), visceral (internal organs) and neuropathic (nerve) causes, as well as the central nervous system processes contributing to these interconnecting systems. We aim to help each child/teenager move, play and feel their body on their journey toward overall wellbeing.


