Women’s Pelvic health
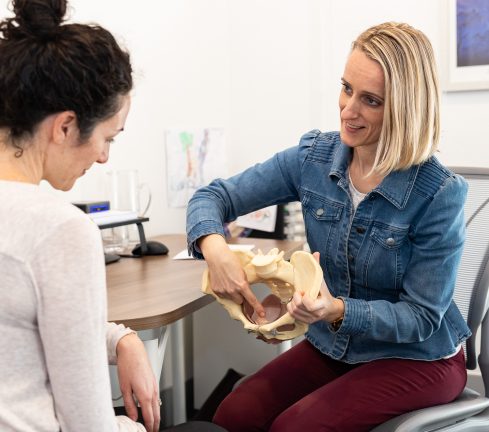
We view the pelvis as the foundation in the body, and of special significance in a woman’s body. Many women find it hard to identify this area of the body, and benefit from individualised assessment and feedback.
We view symptoms, such as bladder leakage and pain, as the body’s way of communicating a need for change. Our pelvic health physios are highly trained and are experienced in helping women learn about their pelvis, and feel all of the different parts – including the pelvic floor muscles. Our physiotherapists have also experienced being pelvic health ‘patients’, and understand what it feels like to be vulnerable in this way.
Pelvic Floor Muscles in Women
Pelvic floor muscles are a complex, small group of muscles found in the base, or ‘floor’, of the bony pelvis.
They are formed from two layers of muscle, originating at the tailbone (coccyx) and spanning outwards and forwards to the front of the pelvis (pubis). The muscles closest to the surface, known collectively as the perineal muscles, form a continuous loop around the vaginal and urethral openings, and the anus. In diagrams, they can appear like a figure of eight, and the muscles work together to close these openings and prevent the (unwanted) passage of urine or faeces.
The deeper pelvic floor muscles, known as the levator ani, work together with the perineals to contain urine and faeces, as well as to support the bladder, vagina and rectum within the pelvis. They are not alone, however, working in a team with other neighbouring muscles and importantly, fascia that is interwoven throughout the pelvis and continuous with muscles and fascia throughout the rest of the body. The unique layout of the pelvic floor muscles in women is vital for allowing normal childbirth, as the baby passes through these muscles to make its way into the world.
What makes pelvic floor muscles especially fascinating, is that they respond not only to our conscious attempts to tighten/release, but to other stimuli. For example, bladder urgency repeatedly causes pelvic floor muscles to tense, sometimes unknowingly. Likewise, pain in the pelvis and other parts of the body can cause pelvic floor muscle tension, over long periods of time. Further, pelvic floor muscles respond to emotions – for example, fear tends to cause these muscles to tense immediately. Anxiety can cause prolonged pelvic floor muscle tension, contributing to pain and problems with bladder, bowel and sexual function.
Pelvic floor muscle training has been demonstrated to be an effective method for improving many pelvic health symptoms, including urinary incontinence, pelvic organ prolapse and pelvic pain. However, pelvic floor muscle training is not the same for every woman. Some women have tight, tense muscles; still others have lower tone, weakened muscles. At Consano our pelvic health practitioners help women to connect with and feel this elusive part of the body. Learning to feel the pelvic floor muscles means they can respond more appropriately to stimuli. Individualised assessment by our practitioners is the pathway to help women to achieve their treatment goals.

Prolapse
Pelvic organ prolapse (POP) is common and will affect up to half of all women who have had a baby.
Prolapse is often described as a bothersome bulge at the vaginal opening, but is so much more. The feeling of prolapse can lead to significant psychological distress.
Many women feel ‘let down’ by their body, and may experience difficulty with exercising, emptying their bladder or bowel, pain and changes in sexual function. Research has demonstrated that specialised pelvic health physiotherapy is effective in the management of prolapse and in particular, strengthening of the pelvic muscles. Our team are skilled in supporting women on this journey and committed to seeking the best possible outcomes.
Bladder problems
Urinary incontinence (UI), or bladder leakage, is perhaps the most commonly recognised women’s pelvic health symptom
Whilst more common after pregnancy and menopause, UI can occur at any age and stage of a woman’s life, for different reasons.
Many women wait years to seek help for this problem, which is often curable. UI can occur with increased abdominal pressure such as coughing, laughing or exercising; with bladder urgency; and with other causes. For many women, pelvic floor muscle training can improve or cure their symptoms; for others, a different approach is required. For these reasons, urinary incontinence requires thorough assessment and individualised management.
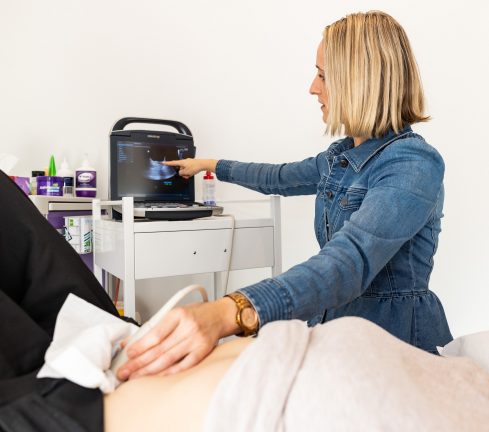
Our pelvic health physios are highly trained in assessing and managing bladder problems in women. We utilise specialised equipment including real-time ultrasound and uroflowmetry, and will refer on for medical assessment and treatment as required. We take delight in seeing women’s symptoms change week by week as they better understand their body, learn to feel their pelvic area, and take action to remedy their own condition.

Bowel problems
Both constipation and faecal incontinence (leakage from the bowel) are more common in women than men.
These problems can be embarrassing, distressing and infuriating and significantly impact a woman’s engagement in normal activities.
Our pelvic health physios take a ‘systems’ approach to managing problems related to the bowel, including biological, nutritional, emotional, myofascial, mechanical, postural, psychological and social contributors. The bowel is such a fascinating part of a woman’s body and deserves a great deal of respect.
As science seeks to better understand the bowel, we remain in touch with current research and practice to remedy and restore improved bowel function.
Pelvic Pain
Pulsing, throbbing, stabbing, aching, burning, splitting, cramping, pressure, tightening.. these are some of the words used by women to describe pain felt in the pelvis and lower abdomen.
Pelvic pain occurs more commonly in women and can be experienced during or after sex, at particular times during the menstrual cycle, with movement, at rest, and throughout the full range of emotions.
The international definition of pain describes both a ‘sensory and emotional’ experience felt in the body.
Our approach to assessing and managing pelvic pain is to consider all of the systems interacting to produce this experience in the body – this is called a biopsychosocial approach.. otherwise known as a holistic approach.
Our team are actively contributing to research into pelvic pain. We are passionate about supporting women to heal, at any age.


Pregnancy
If ever there is a time when women want and need specialised care, it is during pregnancy.
This is the time when the unique functions of a woman’s pelvis are realised, as it becomes the ‘home’ for her growing baby and the pathway to meeting her little one face to face.
Our pelvic health physios support women to understand and adapt to the changes in their bodies during pregnancy and birthing.
- We aim to give women confidence in their own body and it’s amazing abilities.
- We regularly work with women to improve common discomforts including pubic symphysis dysfunction, pelvic girdle pain, lower back pain, constipation/difficult bowel emptying, bladder leakage and vulval varicosities.
- Learning to feel and exercise the pelvic floor muscles during pregnancy can be beneficial for the birth process – for mother and baby – as well as for keeping these muscles strong and supple throughout the pregnancy journey. We work together with women to optimise pelvic health during pregnancy and beyond.
- We provide tailored pregnancy and childbirth education to each woman to support her and her baby to birth normally.
- We help women to understand and connect to ALL the emotions commonly experienced during pregnancy and birth, as we believe this positively impacts a woman’s physiology and physical functioning…and therefore her baby’s.
Postnatal
Also called the ‘postpartum period’ or the fourth trimester, the first year or so after a woman has been pregnant and given birth, is a unique time in her life physically, emotionally and socially.
Our pelvic health physiotherapists support women to remedy symptoms after birth, to restore the most significantly impacted areas, and to return to exercise in a way that works for them. We understand the impact of birth-related trauma on women, their babies and their families. We support women to heal, at their own pace.
- We consider it a privilege to ‘walk alongside’ women during this time.
- We support mothers to breastfeed, and prioritise management of common breastfeeding issues including nipple pain, blocked ducts, mastitis and postural issues related to breastfeeding.
- We provide sensitive and timely management for pain that persists after birth, whether vaginal or Caesarian birth.
- We provide early intervention for pelvic floor trauma associated with birth, including obstetric anal sphincter injury, perineal tears/episiotomy, bladder dysfunction and pelvic organ prolapse.
- We recommend all women have a postnatal pelvic health physio assessment from 6 weeks onward, which includes screening for bladder, bowel, pelvic floor and sexual health issues and provision of an individualised pelvic floor exercise program.
- We expertly assess and manage common musculoskeletal concerns, including rectus abdominis diastasis (RAD/DRA), pelvic floor weakness, abdominal weakness, lumbopelvic pain and wrist pain.


